Calgary
To wear, or not to wear a homemade mask? That is the question.

To do or not to do? That is the question. With my apologies for butchering William Shakespeare’s 1603, Hamlet script from Act 3, Scene 1.
Should I? Should we, wear a homemade mouth and nose masks every time we leave our residence? With so many mixed messages, what to do? It is a simple fact and without question; frontline medical workers and first responders need the store-bought medical masks right now.
Like most, I have had my days consumed by #Covid19 coverage and updates. A Google search of “coronavirus” gave me 6,220,000,000 results back in just 0.58 seconds. A life-time of reading and then some.
One world leader says this, other world leaders says something else. The World Health Organization (WHO) says this, the United Nations (UN) say that. Medical professionals can have conflicting messages from city to city and province to province. Add the stress of watching a virus spread, cratering economies around the world; our heads are spinning with over information.

Canada’s official position backed by Chief Public Health Officer Dr. Theresa Tam, has been strongly against everyone in the country wearing homemade face masks. In a recent press conference Tam said, “What we worry about is actually the potential negative aspects of wearing a mask, where people are not protecting their eyes or other aspects of where the virus could enter your body, and that gives you a false sense of confidence,” and added, “also, it increases the touching of your face. If you think about it, if you’ve got a mask around your face sometimes you can’t help it.”
Canada’s stance aside, in recent days, Western and European countries are starting to join Asian countries’ practises, where the rules for the population are either voluntarily or it’s mandated to wear a face mask in a public setting; some countries with strict penalties. This of course a major U-turn for many countries, considering how there are “Anti-mask laws” in place.

The US Surgeon General, Dr. Jerome Adam in a scene from his “how-to” video on how to make a face mask, with-out sewing.
On April 3rd, US President Donald Trump, announced his administration and the Centers for Disease Control and Prevention (CDC) recommending on a voluntary basis, that Americans wear “non-medical cloth” face coverings. Trump also added that right now he would not partake in the mask wear practise, saying, “Maybe I’ll change my mind.” The Surgeon General, Dr. Jerome Adam posted a “how-to” video on how to make a face mask, with-our sewing.
In the Czech Republic the prime minister, Andrej Babiš has taken a much stronger stance, mandating the covering the nose and mouth at all times outside the home. Aside from closing the boarders and all non-essential businesses, restricting public gatherings, the leader sees the new move as, “vital in controlling the spread of Covid- 19”. The Czech leader has also urged all other governments to follow their lead.
The Czech government became the second country behind Slovakia, in Europe to impose mandatory mask-wearing. No, the Czech government is NOT supplying its 10-million citizens with masks, pharmacies are not selling surgical and medical grade masks to the public, they are for front-line workers.
Without missing a beat and backed by a #Masks4All movement many “how-to” online videos popped-up including one featuring the Minister of Health of, Adam Vojtěch.

Tens of thousands of Czech’s along with businesses nation-wide immediately began churning out homemade masks out of a variety of fabrics. It has been reported that within a short number of days, there was enough for everyone going outside.
Well it turns out, not “everyone” that went outside was wearing a mask. On April 3rd, Czech police were called to a favourite area for nudists. No shirt, no shoes, no pants, no issues, but no face mask, that is a problem! It is not known if any of the sun absorbing naturalists were issued a $800US fine for public disobedience that came along with the Czech government’s new rules.

Czech police were called to a favourite area for nudists. No mask? That is a problem. Photo/Police Czech Republic
As the debate to wear or not circle’s the globe, there is no ignoring that mask wearing countries like, South Korea, Taiwan, Japan and Singapore have not had the horrifying mass outbreaks like those in Italy, Spain, New York now quickly spreading across the US.

Medical staff work wearing proper personal protective equipment (PPE), will there be enough to last through this COVID-19 pandemic? THE CANADIAN PRESS/Justin Tang
There is a worried thought the, “Lull it could give” the population but people know there are still all the other social distancing and sanitation rules. The biggest worry by far is for the front-line medicals workers plus all the first responders. There is a mask shortage now, forcing health workers to disregard basic coronavirus infection control by washing disposable masks and reusing other items already. A mandatory face mask rule could lead to the risking of tens of thousands of people.
No matter voluntary or mandatory, we all must know that medical and 1st responders come first; the general public should wear cloth masks.
Alberta
This is what wasting taxpayer dollars sounds like

From the Canadian Taxpayers Federation
The Canadian Taxpayers Federation is calling on the City of Calgary to scrap the Calgary Arts Development Authority after it spent $65,000 on a telephone line to the Bow River.
“If someone wants to listen to a river, they can go sit next to one, but the City of Calgary should not force taxpayers to pay for this,” said Kris Sims, CTF Alberta Director. “If phoning a river floats your boat, you do you, but don’t force your neighbour to pay for your art choices.”
The City of Calgary spent $65,194 of taxpayers’ money for an art project dubbed “Reconnecting to the Bow” to set up a telephone line so people could call the Bow River and listen to the sound of water.
The project is running between September 2024 and December 2025, according to documents obtained by the CTF.
The art installation is a rerun of a previous version set up back in 2014.
Emails obtained by the CTF show the bureaucrats responsible for the newest version of the project wanted a new local 403 area code phone number instead of an 1-855 number to “give the authority back to the Bow,” because “the original number highlighted a proprietary and commercial relationship with the river.”
Further correspondence obtained by the CTF shows the city did not want its logo included in the displays, stating the “City of Calgary (does NOT want to have its logo on the artworks or advertisements).”
Taxpayers pay about $19 million per year for the Calgary Arts Development Authority. That’s equivalent to the total property tax bill for about 7,000 households.
Calgary bureaucrats also expressed concern the project “may not be received well, perceived as a waste of money or simply foolish.”
“That city hall employee was pointing out the obvious: This is a foolish waste of taxpayers’ money and this slush fund should be scrapped,” said Sims. “Artists should work with willing donors for their projects instead of mooching off city hall and forcing taxpayers to pay for it.”
Alberta
Scotia Place – Calgary unveils design for new arena / events centre

News release from the City of Calgary
Scotia Place, Calgary’s new event centre, designed as a place for community where there is room for everyone
The City of Calgary and Calgary Sports and Entertainment Corporation (CSEC) are excited to reveal the design for Calgary’s new event centre – formally named Scotia Place.
The design is influenced by the ancestral and historical land of Indigenous Peoples and the culturally significant site that embodies our shared purpose – to gather. It brings together Indigenous cultural perspectives with Calgary’s and the region’s natural beauty, reflecting the four elements of nature – fire, ice, land and air.
A striking feature of the building is the central structure with a textured flame motif that emulates a home fire, which is further amplified when it is lit at night. The home fire, a place of warmth and energy that brings people together to share stories of the past and create stories for the future, rises from the white, glacial-like forms that define the lower parts of the building.
“When you consider that Calgary is already the envy of other cities with a new world-class convention centre in the heart of the Culture + Entertainment District, the addition of Scotia Place is another signal to investors that our city understands how to build a future that leverages hospitality and hosting as its core strengths,” says Mayor Jyoti Gondek. “We are also acknowledging and honouring the foundational role that Indigenous communities have played for generations in making Calgary, and now Scotia Place, a space where we all belong.”
Scotia Place, which is scheduled to open in fall 2027, celebrates the area’s importance as a place for all and will be a landmark attraction in Calgary’s emerging Culture + Entertainment District. More than a building, however, the 10-acre city block is designed for community and connection and includes a community rink, outdoor and indoor plazas spaces, four restaurants, the Calgary Flames Team Store, and future development opportunity in the northeast corner. It will provide gathering places and amenities for the 8,000 people who will live in this new downtown neighbourhood.
“Calgary has a long history of hosting world-class events, drawing millions of visitors to the city each year, generating revenue for local businesses, and boosting the economy,” says Danielle Smith, Premier of the Province of Alberta. “With construction on the Calgary Rivers District and Event Centre now underway, Calgary is one step closer to a revitalized downtown that will bring new energy into the city, attract more exciting events, and create jobs to improve the quality of life for Calgarians.”
A development permit application for the facility was submitted on July 19, 2024. This was a significant milestone for the project team, consisting of CAA ICON, HOK-DIALOG, and CANA/Mortenson. People interested in following or commenting on the permit can find the application at Calgary.ca/dmap. The application is expected to be heard by the Calgary Planning Commission by end of 2024.
“This is an important day for Calgary,” says Councillor Sonya Sharp, Event Centre Committee Chair. “Today is about so much more than the designs of a building. Today is the unveiling of a place where Calgarians and visitors from around the world will make memories at concerts, and sport and community events. I hope that everyone is as excited as we are, knowing that Scotia Place will become the complete experience in our new Culture & Entertainment District.”
“At CSEC, a key component of our mission is to be the heartbeat of our community, create connections and bring people together,” said Robert Hayes, CSEC President and CEO. “Scotia Place will become the perfect home to achieve and share this mission with all Calgarians. Seeing the design brings the vision of so many contributors to life. We are especially thankful to the City of Calgary and the Province of Alberta for their leadership and support to help bring us to this point. In stride with our partner Scotiabank, we are very proud to play our role in presenting Scotia Place as the culmination of diligence and passion, that is now visual in this breathtakingly beautiful and meaningful facility.”
“For years we have seen firsthand the value these partnerships bring to the communities in which we operate and for our clients,” said Aris Bogdaneris, Group Head, Canadian Banking of Scotiabank. “Scotia Place introduces a bold new vision for what will be Alberta’s premier sports and entertainment venue. For nearly 20 years, Scotiabank has been a proud partner of Calgary Sports and Entertainment Corporation and together, we are committed to bring fans and our clients an unforgettable experience when they walk through the doors of Scotia Place.”
“We are excited to start the construction of the critical infrastructure needed to build thousands of new homes and to make the Calgary’s new Culture + Entertainment district a reality,” says Devin Dreeshen, Minister of Transportation and Economic Corridors. “Albertans expect basic infrastructure to be maintained and improved and this commitment from the province goes a long way in helping Calgary build these projects.”
Acknowledging the significance of the building’s location at the confluence of the Bow and Elbow Rivers on the ancestral land of the Treaty 7 Peoples and the Metis Nation, The City, CSEC, HOK-DIALOG and CAA ICON worked with an Indigenous Advisory Group that included representatives from the Treaty 7 Nations, the Métis Nation of Alberta, Region 3, and the Urban Indigenous community throughout the design process.
“It was great to be part of a truly representative voice that included all indigenous peoples of southern Alberta regarding the design of this center acknowledging the historic significance of the land it sits on to the Metis people,” said Carmen Lasante Captain of the Calgary Elbow Metis District. “Inclusivity is a core part of who the Metis are. The City has worked hard to include many diverse histories together in creating this space.”
“Engaging in the right way is fundamental to the success of relationship development with the Indigenous communities, as we have played a critical role in the identity of the land now known as the city of Calgary as the Indigenous nations are inextricable linked to the landscape and environment,” says Ira Provost, Piikani Nation Consultation
A key theme heard often during the Indigenous engagement sessions was “Come in, there is room”, making it clear that Scotia Place needs to be a place that is designed for all.
The public plazas are designed to honour the deep-rooted connection that Indigenous Peoples have with the land, incorporating representations of the tipi, Métis Trapper’s Tent, and elements of Alberta’s world-renown natural landscape.
An important design decision was to lower the event and ice surface so that the primary concourse will be at street-level. Calgarians and visitors will be able to move seamlessly between the curb, the primary concourse and the outdoor public plazas.
“We at DIALOG are thrilled to join forces with HOK and combine our unique expertise to transform Calgary’s Event Centre into the catalyst for a dynamic new urban community,” says Doug Cinnamon, Partner Architect at DIALOG.
“Other design principles including public realm activation, the integration of indigenous influences, public art & storytelling, sustainability, and a balance between past, present, and future is central to our vision. The ultimate goal is to ensure seamless accessibility, promote mixed uses, and create vibrant public areas for everyone to enjoy. This joint redesign represents an opportunity to spur investment into the area and enhance its cultural vitality, anchoring Calgary’s position as a thriving, bustling community hub.”
Scotia Place is a generational investment in Calgary’s emerging vibrant Culture + Entertainment District. A modern event centre with universal accessible design throughout and with energy and water conservation built in to maximize efficiencies and the ability to be net-zero by 2050, Scotia place is designed to serve Calgary’s growing community for decades to come.
Construction begins this week. Additional information about Scotia Place including design renderings, a video, and frequently asked questions is available on Calgary.ca/ScotiaPlace.
-

 Alberta10 hours ago
Alberta10 hours agoAlberta Independence Seekers Take First Step: Citizen Initiative Application Approved, Notice of Initiative Petition Issued
-
 Crime9 hours ago
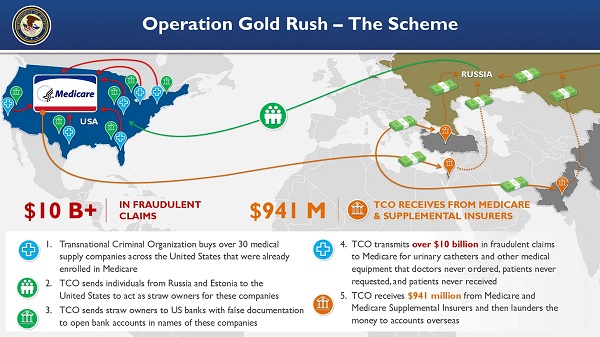
Crime9 hours agoNational Health Care Fraud Takedown Results in 324 Defendants Charged in Connection with Over $14.6 Billion in Alleged Fraud
-

 Health8 hours ago
Health8 hours agoRFK Jr. Unloads Disturbing Vaccine Secrets on Tucker—And Surprises Everyone on Trump
-

 Bruce Dowbiggin11 hours ago
Bruce Dowbiggin11 hours agoThe Game That Let Canadians Forgive The Liberals — Again
-

 Alberta1 day ago
Alberta1 day agoCOVID mandates protester in Canada released on bail after over 2 years in jail
-

 Crime2 days ago
Crime2 days agoProject Sleeping Giant: Inside the Chinese Mercantile Machine Linking Beijing’s Underground Banks and the Sinaloa Cartel
-

 Alberta2 days ago
Alberta2 days agoAlberta uncorks new rules for liquor and cannabis
-

 Business1 day ago
Business1 day agoCanada’s loyalty to globalism is bleeding our economy dry