Addictions
News For Those Who Think Drug Criminalization Is Racist. Minorities Disagree

A Canadian poll finds that racial minorities don’t believe drug enforcement is bigoted.
By Adam Zivo
[This article was originally published in City Journal, a public policy magazine and website published by the Manhattan Institute for Policy Research]
Is drug prohibition racist? Many left-wing institutions seem to think so. But their argument is historically illiterate—and it contradicts recent polling data, too, which show that minorities overwhelmingly reject that view.
Policies and laws are tools to establish order. Like any tool, they can be abused. The first drug laws in North America, dating back to the late nineteenth and early twentieth centuries, arguably fixated on opium as a legal pretext to harass Asian immigrants, for example. But no reasonable person would argue that laws against home invasion, murder, or theft are “racist” because they have been misapplied in past cases. Absent supporting evidence, leaping from “this tool is sometimes used in racist ways” to “this tool is essentially racist” is kindergarten-level reasoning.
Yet this is precisely what institutions and activist groups throughout the Western world have done. The Drug Policy Alliance, a U.S.-based organization, suggests that drug prohibition is rooted in “racism and fear.” Harm Reduction International, a British NGO, argues for legalization on the grounds that drug prohibition entrenches “racialized hierarchies, which were established under colonial control and continue to dominate today.” In Canada, where I live, the top public health official in British Columbia, our most drug-permissive province, released a pro-legalization report last summer claiming that prohibition is “based on a history of racism, white supremacy, paternalism, colonialism, classism and human rights violations.”
These claims ignore how drug prohibition has been and remains popular in many non-European societies. Sharia law has banned the use of mind-altering substances since the seventh century. When Indigenous leaders negotiated treaties with Canadian colonists in the late 1800s, they asked for “the exclusion of fire water (whiskey)” from their communities. That same century, China’s Qing Empire banned opium amid a national addiction crisis. “Opium is a poison, undermining our good customs and morality,” the Daoguang emperor wrote in an 1810 edict.
Today, Asian and Muslim jurisdictions impose much stiffer penalties on drug offenders than do Western nations. In countries like China, Saudi Arabia, Iran, Singapore, and Thailand, addicts and traffickers are given lengthy prison sentences or executed. Meantime, in Canada and the United States, de facto decriminalization has left urban cores littered with syringes and shrouded in clouds of meth.
The anti-drug backlash building in North America appears to be spearheaded by racial minorities. When Chesa Boudin, San Francisco’s former district attorney, was recalled in 2022, support for his ouster was highest among Asian voters. Last fall, 73 percent of Latinos backed California’s Proposition 36, which heightened penalties for drug crimes, while only 58 percent of white respondents did.
In Canada, the first signs of a parallel trend emerged during Vancouver’s 2022 municipal election, where an apparent surge in Chinese Canadian support helped install a slate of pro-police candidates. Then, in British Columbia’s provincial election last autumn, nonwhite voters strongly preferred the BC Conservatives, who campaigned on stricter drug laws. And in last month’s federal election, within both Vancouver and Toronto’s metropolitan areas, tough-on-crime conservatives received considerable support from South Asian communities.
These are all strong indicators that racial minorities do not, in fact, universally favor drug legalization. But their small population share means there is relatively little polling data to measure their preferences. Since only 7.6 percent of Americans are Asian, for example, a poll of 1,000 randomly selected people will yield an average of only 76 Asian respondents—too small a sample from which to draw meaningful conclusions. You can overcome this barrier by commissioning very large polls, but that’s expensive.
Nonetheless, last autumn, the Centre for Responsible Drug Policy (a nonprofit I founded and operate) did just that. In partnership with the Macdonald-Laurier Institute, we contracted Mainstreet Research to ask over 12,000 British Columbians: “Do you agree or disagree that criminalizing drugs is racist?”
The results undermine progressives’ assumptions. Only 26 percent of nonwhite respondents agreed (either strongly or weakly) that drug criminalization is racist, while over twice as many (56 percent) disagreed. The share of nonwhite respondents who strongly disagreed was three times larger than the share that strongly agreed (43.2 percent versus 14.3 percent). These results are fairly conclusive for this jurisdiction, given the poll’s sample size of 2,233 nonwhite respondents and a margin of error of 2 percent.
Notably, Indigenous respondents seemed to be the most anti-drug ethnic group: only 20 percent agreed (weakly or strongly) with the “criminalization is racist” narrative, while 61 percent disagreed. Once again, those who disagreed were much more vehement than those who agreed. With a sample size of 399 respondents, the margin of error here (5 percent) is too small to confound these dramatic results.
We saw similar outcomes for other minority groups, such as South Asians, Southeast Asians, Latinos, and blacks. While Middle Eastern respondents also seemed to follow this trend, the poll included too few of them to draw definitive conclusions. Only East Asians were divided on the issue, though a clear majority still disagreed that criminalization is racist.
As this poll was limited to British Columbian respondents, our findings cannot necessarily be assumed to hold throughout Canada and the United States. But since the province is arguably the most drug-permissive jurisdiction within the two countries, these results could represent the ceiling of pro-drug, anti-criminalization attitudes among minority communities.
Legalization proponents and their progressive allies take pride in being “anti-racist.” Our polling, however, suggests that they are not listening to the communities they profess to care about.
Our content is always free – but if you want to help us commission more high-quality journalism,
please consider getting a voluntary paid subscription.
Addictions
New RCMP program steering opioid addicted towards treatment and recovery

News release from Alberta RCMP
Virtual Opioid Dependency Program serves vulnerable population in Red Deer
Since April 2024, your Alberta RCMP’s Community Safety and Well-being Branch (CSWB) has been piloting the Virtual Opioid Dependency Program (VODP) program in Red Deer to assist those facing opioid dependency with initial-stage intervention services. VODP is a collaboration with the Government of Alberta, Recovery Alberta, and the Alberta RCMP, and was created to help address opioid addiction across the province.
Red Deer’s VODP consists of two teams, each consisting of a police officer and a paramedic. These teams cover the communities of Red Deer, Innisfail, Blackfalds and Sylvan Lake. The goal of the program is to have frontline points of contact that can assist opioid users by getting them access to treatment, counselling, and life-saving medication.
The Alberta RCMP’s role in VODP:
- Conducting outreach in the community, on foot, by vehicle, and even UTV, and interacting with vulnerable persons and talking with them about treatment options and making VODP referrals.
- Attending calls for service in which opioid use may be a factor, such as drug poisonings, open drug use in public, social diversion calls, etc.
- Administering medication such as Suboxone and Sublocade to opioid users who are arrested and lodged in RCMP cells and voluntarily wish to participate in VODP; these medications help with withdrawal symptoms and are the primary method for treating opioid addiction. Individuals may be provided ongoing treatment while in police custody or incarceration.
- Collaborating with agencies in the treatment and addiction space to work together on client care. Red Deer’s VODP chairs a quarterly Vulnerable Populations Working Group meeting consisting of a number of local stakeholders who come together to address both client and community needs.
While accountability for criminal actions is necessary, the Alberta RCMP recognizes that opioid addiction is part of larger social and health issues that require long-term supports. Often people facing addictions are among offenders who land in a cycle of criminality. As first responders, our officers are frequently in contact with these individuals. We are ideally placed to help connect those individuals with the VODP. The Alberta RCMP helps those individuals who wish to participate in the VODP by ensuring that they have access to necessary resources and receive the medical care they need, even while they are in police custody.
Since its start, the Red Deer program has made nearly 2,500 referrals and touchpoints with individuals, discussing VODP participation and treatment options. Some successes of the program include:
- In October 2024, Red Deer VODP assessed a 35-year-old male who was arrested and in police custody. The individual was put in contact with medical care and was prescribed and administered Suboxone. The team members did not have any contact with the male again until April 2025 when the individual visited the detachment to thank the team for treating him with care and dignity while in cells, and for getting him access to treatment. The individual stated he had been sober since, saying the treatment saved his life.
- In May 2025, the VODP team worked with a 14-year-old female who was arrested on warrants and lodged in RCMP cells. She had run away from home and was located downtown using opioids. The team spoke to the girl about treatment, was referred to VODP, and was administered Sublocade to treat her addiction. During follow-up, the team received positive feedback from both the family and the attending care providers.
The VODP provides same-day medication starts, opioid treatment transition services, and ongoing opioid dependency care to people anywhere in Alberta who are living with opioid addiction. Visit vodp.ca to learn more.
“This collaboration between Alberta’s Government, Recovery Alberta and the RCMP is a powerful example of how partnerships between health and public safety can change lives. The Virtual Opioid Dependency Program can be the first step in a person’s journey to recovery,” says Alberta’s Minister of Mental Health and Addiction Rick Wilson. “By connecting people to treatment when and where they need it most, we are helping build more paths to recovery and to a healthier Alberta.”
“Part of the Alberta RCMP’s CSWB mandate is the enhancement of public safety through community partnerships,” says Supt. Holly Glassford, Detachment Commander of Red Deer RCMP. “Through VODP, we are committed to building upon community partnerships with social and health agencies, so that we can increase accessibility to supports in our city and reduce crime in Red Deer. Together we are creating a stronger, safer Alberta.”
Addictions
Saskatchewan launches small fleet of wellness buses to expand addictions care

By Alexandra Keeler
Across Canada, mobile health models are increasingly being used to offer care to rural and underserved communities
Saskatchewan has launched a small fleet of mobile wellness buses to improve access to primary health care, mental health and addiction services in the province.
The first bus began operating in Regina on Feb. 12. Another followed in Prince Albert on March 21. Saskatoon’s bus was unveiled publicly on April 9. All three are former coach buses that have been retrofitted to provide health care to communities facing barriers to access.
“Mobile health units are proven to improve outcomes for people facing barriers to healthcare,” Kayla DeMong, the executive director of addiction treatment centre Prairie Harm Reduction, told Canadian Affairs in an email.
“We fully support this innovative approach and are excited to work alongside the health bus teams to ensure the people we support receive the care they need, when and where they need it.”
Wellness buses
Like all provinces, Saskatchewan has been grappling with the opioid crisis.
In 2023, an estimated 457 individuals died from overdoses in the province. In 2024, that number fell to 346. But the province continues to struggle with fatal and non-fatal overdoses.
In late February, Saskatoon firefighters responded to more than 25 overdoses in a single 24-hour period. Just over a week later, they responded to 37 overdoses within another 24-hour window.
Saskatchewan’s wellness buses are part of the province’s plan to address these problems. In April 2025, the province announced $2.4 million to purchase and retrofit three coach buses, plus $1.5 million in annual operating funds.
The buses operate on fixed schedules at designated locations around each city. Each bus is staffed with a nurse practitioner, nurse and assessor coordinator who offer services such as overdose reversal kits, addiction medicine and mental health referrals.
“By bringing services directly to where people are, the health buses foster safer, more welcoming spaces and help build trusting relationships between community members and care providers,” said DeMong, executive director of Prairie Harm Reduction.
Saskatoon-based Prairie Harm Reduction is one of the local organizations that partners with the buses to provide additional support services. Prairie Harm Reduction provides a range of family, youth and community supports, and also houses the province’s only fixed supervised consumption site.
The mobile model
Saskatchewan is not the only province using wellness buses. Across Canada, mobile health models are increasingly being used to expand access to care in rural and underserved communities.
In Kingston, Ont., the Street Health Centre operates a retrofitted RV called PORCH (Portable Outreach Care Hub) that serves individuals struggling with homelessness and addiction.
“Our outreach services are extremely popular with our clients and community partners,” Donna Glasspoole, manager at Street Health Centre, said in an emailed statement.
“PORCH hits the road two to three days/week and offers a variety of services, which are dependent on the health care providers and community partners aboard.”
Street Health Centre also has a shuttle service that picks up clients in shelters and brings them to medical clinics or addiction medicine clinics.
The PORCH vehicles are not supported by provincial funding, but instead rely on support from the United Way and other grants. Glasspoole says the centre’s permanent location — which does receive government funding — is more cost-effective to operate.
“The vehicles are expensive to operate and our RV is not great in winter months and requires indoor parking,” she said.

Politically palatable
Many mobile health models currently do not provide controversial services such as supervised drug consumption.
The Saskatchewan Health Authority told Canadian Affairs the province’s new wellness buses will not offer supervised consumption services or safer supply, where drug users are given prescribed opioids as an alternative to toxic street drugs.
“There are no plans to provide supervised consumption services from the wellness buses,” Saskatchewan Health Authority spokesperson Courtney Markewich told Canadian Affairs in a phone call.
This limited scope may make mobile services more politically palatable in provinces that have resisted harm reduction measures.
In Ontario, some harm reduction programs have shifted to mobile models following Premier Doug Ford’s decision to suspend supervised consumption services located within 200 metres of schools and daycares.
In April, Toronto Public Health ended operations at its Victoria Street fixed consumption site, replacing it with street outreach and mobile vans.
The Ontario government’s decision to close the sites is part of a broader pivot away from harm reduction. The province is investing $378 million to transition suspended sites into 19 new “HART Hubs” that offer primary care, mental health, addictions treatment and other supports.
Glasspoole says that what matters most is not whether services are provided at fixed or mobile locations, but how care is delivered.
Models that “reduce barriers to care, [are] non-judgemental, and [are staffed by] trauma-informed providers” are what lead more people toward treatment and recovery, she said in her email.
In Saskatchewan, DeMong hopes the province’s new wellness buses help address persistent service gaps and build trust with underserved communities.
“This initiative is a vital step toward filling long-standing gaps in the continuum of care by providing low-barrier, community-based access to health-care services,” she said.
This article was produced through the Breaking Needles Fellowship Program, which provided a grant to Canadian Affairs, a digital media outlet, to fund journalism exploring addiction and crime in Canada. Articles produced through the Fellowship are co-published by Break The Needle and Canadian Affairs.
Subscribe to Break The Needle
-

 Alberta7 hours ago
Alberta7 hours agoAlberta Independence Seekers Take First Step: Citizen Initiative Application Approved, Notice of Initiative Petition Issued
-
 Crime6 hours ago
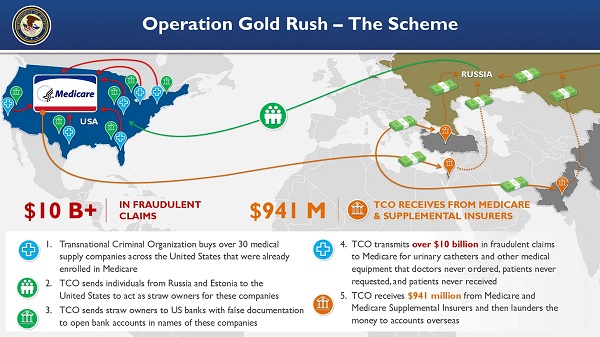
Crime6 hours agoNational Health Care Fraud Takedown Results in 324 Defendants Charged in Connection with Over $14.6 Billion in Alleged Fraud
-

 Health5 hours ago
Health5 hours agoRFK Jr. Unloads Disturbing Vaccine Secrets on Tucker—And Surprises Everyone on Trump
-

 Bruce Dowbiggin8 hours ago
Bruce Dowbiggin8 hours agoThe Game That Let Canadians Forgive The Liberals — Again
-

 Agriculture2 days ago
Agriculture2 days agoCanada’s supply management system is failing consumers
-

 Alberta1 day ago
Alberta1 day agoCOVID mandates protester in Canada released on bail after over 2 years in jail
-

 Crime2 days ago
Crime2 days agoProject Sleeping Giant: Inside the Chinese Mercantile Machine Linking Beijing’s Underground Banks and the Sinaloa Cartel
-

 Alberta1 day ago
Alberta1 day agoAlberta uncorks new rules for liquor and cannabis