Community
ALCOHOLISM-THE GIFT OF KNOWLEDGE WE CAN GIVE OUR CHILDREN

A few weeks ago, celebrity Ben Affleck had the media going wild. While most people go to great lengths and efforts to hide the truth, he did the unthinkable—he publicly announced that he has recently completed treatment for alcoholism.
What I found even more remarkable, courageous, and important is that he went even further and said, “I want to live life to the fullest and be the best father I can be. I want my kids to know there is no shame in getting help when you need it, and to be a source of strength for anyone out there who needs help but is afraid to take that first step.”
What?! He told his children!?
I am the adult child of an alcoholic. Otherwise known as ACOA. I have known what that word meant since I was five years old, but not because anyone told me. Families keep secrets and mine is no different. Or should I say, families think they keep secrets but, even as little children, we figure things out very quickly.
Adults may think they are hiding what is going on around their children. But they are not. Kids are like little sponges; interpreting, analyzing, and absorbing. All that adults are doing is not realizing that the little underdeveloped brains of three-, five-, and ten-year-olds are putting together the little puzzle pieces. The things that through osmosis often scare and confuse us can have lasting effects, and sometimes become our lessons of right, not our lessons of wrong.
By the time I was six years old, I had already set my life’s plan into motion with my feet planted firmly on the ground. This alcohol-fueled life my parents had was never going to be mine. Never. I could not have been more wrong. You see, I was not an only child.
ga('create', 'UA-83785338-1', 'auto'); ga('send', 'pageview');
I have been surrounded by alcoholism my whole life—I am the daughter, step-daughter, granddaughter, niece, great-niece, aunt, and cousin to alcoholics. Nothing affected me more than when my younger brother Brett became another branch on our alcoholic family tree; this added “sister” to the long list that follows my name.
Our parents loved us and didn’t beat my brother and me, but understanding more about addiction now and knowing some of its causes, I know we received the scars. Those painful, traumatic experiences changed who we would be forever. I would become strong, stoic, loud, and able to take on the world. At first glance, those things seem like great attributes to have, and although they afforded me the ability to survive the challenges in my life, my feelings of responsibility for the members of my own family almost destroyed me.
Ben Affleck gave his children a gift. The gift of knowledge. The gift of understanding. The gift of truth without shame. And I intend to do the same.
My sweet, kind, soft-spoken, magnificent brother lost his battle with alcoholism in March 2012. My own parents have never acknowledged our past—one remains silent and the other goes so far as to diminish and deny my experiences that continues to cause unnecessary pain more than forty years later.
This was the 1970s. It wouldn’t have been a reasonable expectation to have these open discussions back then and I accept that. But I can’t help wonder if things might have turned out differently if we had worked through some of this in our adult lives. After all, it is amazing what a simple, “I am sorry. I love you” can accomplish.
But we can’t go back, life is about moving forward. My perspective is that I am blessed and proud to be part of a changing world where addiction is a disease and we are encouraged to speak openly and honestly about it. And I believe that starts with young children.
I know all too well, because I was that little girl once, that we overhear those whispers, and although you don’t tell us directly the message is loud and clear, “alcoholism is shameful and you hide it at all costs.” If we truly want to be a part of a changing world, we need to begin the conversation in our own homes, without shame. No one will ever find the courage to speak publicly if we can’t even speak privately in our own families.
My beautiful niece, Kaddi, was only six years old when her beloved uncle died; and I have spoken to her about his passing almost from that very day. Of course, I am careful because she is just a young girl; I share more and more with her each year so she grows up being aware, knowing that addiction and mental illness is in our family. I want her to be as comfortable with understanding the disease of alcoholism as she is with the knowledge that her grandmother (her dad’s mom) passed away before she was born from breast cancer. My niece is eleven years old now, and just a few weeks ago, as she continues putting together all the little puzzle pieces in her mind, she asked me, “Auntie, can girls grow up and become alcoholics?”
“Yes, they can, honey. Yes, they can.”
Jodee Prouse is a speaker and advocate surrounding addiction and mental illness from a family perspective. As well as empowering women that are emerging from challenges with family, sharing her story to give them courage, strength and hope. She is the author of the powerful memoir, THE SUN IS GONE: A Sister Lost in Secrets, Shame, and Addiction, and How I Broke Free.
Visit jodeeprouse.com or email [email protected]
Community
Support local healthcare while winning amazing prizes!
|
|
|
|
|
|
Community
The 2025 Red Deer Hospital Lottery is here! Lower ticket prices!!

|
|
|
|
|
|
-

 Agriculture2 days ago
Agriculture2 days agoCanada’s supply management system is failing consumers
-

 Business1 day ago
Business1 day agoCanada’s loyalty to globalism is bleeding our economy dry
-

 Alberta1 day ago
Alberta1 day agoCOVID mandates protester in Canada released on bail after over 2 years in jail
-

 armed forces1 day ago
armed forces1 day agoCanada’s Military Can’t Be Fixed With Cash Alone
-

 Alberta1 day ago
Alberta1 day agoAlberta Next: Alberta Pension Plan
-

 International1 day ago
International1 day agoTrump transportation secretary tells governors to remove ‘rainbow crosswalks’
-

 Business1 day ago
Business1 day agoCarney’s spending makes Trudeau look like a cheapskate
-

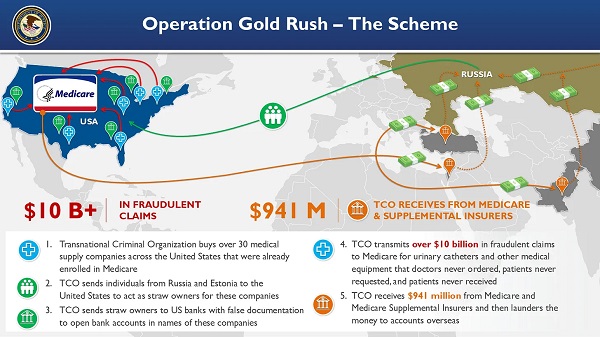
 Crime2 days ago
Crime2 days agoProject Sleeping Giant: Inside the Chinese Mercantile Machine Linking Beijing’s Underground Banks and the Sinaloa Cartel