Health
Dr. Malone: Bird flu ‘emergency’ in California is a case of psychological bioterrorism
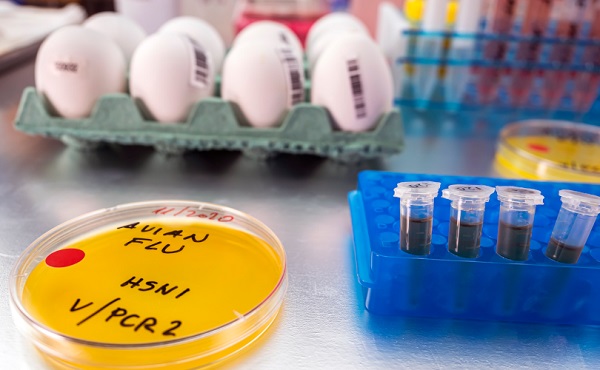
From LifeSiteNews
Contrary to initial reporting from corporate media, the WHO, and the apocalyptic mutterings of Dr. Peter Hotez, there continues to be no evidence indicating the circulation of a highly pathogenic version of bird flu in either animal or human populations.
What is the current threat assessment for Avian Influenza, and has it changed?
I previously established and published a brief baseline threat assessment for Avian Influenza on July 2, 2024. Four dominant parameters must be considered when assessing a potential infectious disease threat to human populations:
- Disease severity (a measurable objective truth)
- Mechanism of transmission and observed transmissibility (an experimentally testable objective truth)
- Evidence of sustained human-to-human transmission (a measurable objective truth)
- Assessment of anticipated future risk (subjective, speculative, and hypothetical)
Politicians and their allies (in BioPharma, academia, and other sectors) have a variety of conflicts of interest and agendas which are not aligned with objective, dispassionate assessment and response to public health and infectious disease issues, and cannot be relied upon to analyze and respond to these key parameters objectively.
An assessment of the conflicts of interest and political agenda(s) of California’s Gavin Newsom is beyond the scope of this analysis. Still, please remember that Governor Newsom clearly mismanaged and overreacted to the COVID threat, as did the World Economic Forum that trained and coached (coaches?) him as a “Young Leader” and clearly continues to influence his political postures.
Although California has remained under Democrat party control – in significant part consequent to “rank choice” voting policies – during the recent presidential election there was a clear shift and momentum toward the Republican party across the majority of the state.
California has a very large dairy industry, and I know that a leader in and representative of that industry has close connections to Newsom. The presence of the virus in Southern California dairy farms is widespread, with over 300 dairy herds testing positive in the last 30 days
Has the threat assessment circa July 2024 changed? Let’s revisit the basics:
Disease severity, December 2024
Disease severity continues to be mild, with the exception of one new case which apparently triggered Newsom to declare a state of emergency in California.
According to Newsweek, “A person in Louisiana was hospitalized in critical condition with severe respiratory symptoms from a bird flu infection, according to state health officials. The patient had been in contact with sick and dead birds in a backyard flock, according to the CDC. Louisiana health officials said the patient is older than 65 and has underlying medical conditions.”
Here is the current CDC threat summary
- H5 bird flu is widespread in wild birds worldwide and is causing outbreaks in poultry and U.S. dairy cows with several recent human cases in U.S. dairy and poultry workers.
- While the current public health risk is low, CDC is watching the situation carefully and working with states to monitor people with animal exposures.
- CDC is using its flu surveillance systems to monitor for H5 bird flu activity in people.



The CDC charts above document that the risk of H5 in humans is low, disease severity is low, and although massive testing has occurred, there are only 61 total “exposure” sources found from cattle, birds, and other mammals.
There are a total of three human cases picked up from the CDC flu surveillance program since February 25, 2024, and a total of 58 cases in the U.S., after testing almost 10,000 people who were exposed to infected animals.
In sum, the profile of disease severity has not changed since July 2024. As opposed to initial reporting from corporate media, dark warnings from the WHO and Dr. Tedros, and the apocalyptic mutterings of Dr. Peter Hotez, there continues to be no evidence indicating the circulation of a highly pathogenic version of this virus in either animal or human populations.
Mechanism of transmission and observed transmissibility
All reported U.S. transmission events involve human exposure in the context of intensive contact during animal husbandry or other known animal hosts, indicating that the mechanism of transmission remains intensive exposure to infected animals and animal carcasses. No change from July 2024.
Evidence of sustained human-to-human transmission
No evidence of sustained human-to-human transmission, now or in the past with this currently circulating variant.
Assessment of anticipated future risk
This appears to be the crux of Newsom’s alarmist response involving the declaration of a “State of Emergency” for bird flu in California. A statement from the governor’s office characterized the move as a “proactive action to strengthen robust state response” to avian influenza A (H5N1), also known as bird flu.
“This proclamation is a targeted action to ensure government agencies have the resources and flexibility they need to respond quickly to this outbreak,” Newsom said in a statement. “Building on California’s testing and monitoring system – the largest in the nation – we are committed to further protecting public health, supporting our agriculture industry, and ensuring that Californians have access to accurate, up-to-date information.”
He added, “While the risk to the public remains low, we will continue to take all necessary steps to prevent the spread of this virus.”
This statement demonstrates either a profound ignorance of the mechanism by which animal influenza viruses spread, including avian influenza, or the presence of a hidden agenda. With a wide range of animal reservoirs, including migratory waterfowl, there is no way that the state of California can prevent the spread of this virus.
READ: Australian doctor who criticized COVID jabs has his suspension reversed
Conclusion
There has been no significant change in the current threat assessment associated with Avian Influenza relative to July 2024. The CDC, which has recently been implicated in industrial-scale “PsyWar” deployment of psychological bioterrorism regarding COVID and has an organizational conflict of interest in promoting vaccines and vaccine uptake, characterizes the current public health risk as low.
My conclusion regarding the Newsom declaration of a “State of Emergency” for bird flu in California is that it is being driven by a hidden agenda. There are multiple hypotheses regarding what that hidden agenda may be, but Newsom’s statement that, “Building on California’s testing and monitoring system – the largest in the nation – we are committed to further protecting public health, supporting our agriculture industry, and ensuring that Californians have access to accurate, up-to-date information,” suggests that this declaration may, at a minimum, reflect advocacy by and for California’s infectious disease testing industry, which includes both academic and commercial components.
Reprinted with permission from Robert Malone.
Addictions
Canada is divided on the drug crisis—so are its doctors

When it comes to addressing the national overdose crisis, the Canadian public seems ideologically split: some groups prioritize recovery and abstinence, while others lean heavily into “harm reduction” and destigmatization. In most cases, we would defer to the experts—but they are similarly divided here.
This factionalism was evident at the Canadian Society of Addiction Medicine’s (CSAM) annual scientific conference this year, which is the country’s largest gathering of addiction medicine practitioners (e.g., physicians, nurses, psychiatrists). Throughout the event, speakers alluded to the field’s disunity and the need to bridge political gaps through collaborative, not adversarial, dialogue.
This was a major shift from previous conferences, which largely ignored the long-brewing battles among addiction experts, and reflected a wider societal rethink of the harm reduction movement, which was politically hegemonic until very recently.
Recovery-oriented care versus harm reductionism
For decades, most Canadian addiction experts focused on shepherding patients towards recovery and encouraging drug abstinence. However, in the 2000s, this began to shift with the rise of harm reductionism, which took a more tolerant view of drug use.
On the surface, harm reductionists advocated for pragmatically minimizing the negative consequences of risky use—for example, through needle exchanges and supervised consumption sites. Additionally, though, many of them also claimed that drug consumption is not inherently wrong or shameful, and that associated harms are primarily caused not by drugs themselves but by the stigmatization and criminalization of their use. In their view, if all hard drugs were legalized and destigmatized, then they would eventually become as banal as alcohol and tobacco.
The harm reductionists gained significant traction in the 2010s thanks to the popularization of street fentanyl. The drug’s incredible potency caused an explosion of deaths and left users with formidable opioid tolerances that rendered traditional addiction medications, such as methadone, less effective. Amid this crisis, policymakers embraced harm reduction out of an immediate need to make drug use slightly less lethal. This typically meant supervising consumption, providing sterile drug paraphernalia, and offering “cleaner” substances for addicts to use.
Many abstinence-oriented addiction experts supported some aspects of harm reduction. They valued interventions that could demonstrably save lives without significant tradeoffs, and saw them as both transitional and as part of a larger public health toolkit. Distributing clean needles and Naloxone, an overdose-reversal medication, proved particularly popular. “People can’t recover if they’re dead,” went a popular mantra from the time.
Saving lives or enabling addiction?
However, many of these addiction experts were also uncomfortable with the broader political ideologies animating the movement and did not believe that drug use should be normalized. Many felt that some experimental harm reduction interventions in Canada were either conceptually flawed or that their implementation had deviated from what had originally been promised.
Some argued, not unreasonably, that the country’s supervised consumption sites are being mismanaged and failing to connect vulnerable addicts to recovery-oriented care. Most of their ire, however, was directed at “safer supply”—a novel strategy wherein addicts are given free drugs, predominantly hydromorphone (a heroin-strength opioid), without any real supervision.
While safer supply was meant to dissuade recipients from using riskier street drugs, addiction physicians widely reported that patients were selling their free hydromorphone to buy stronger illicit fentanyl, thereby flooding communities with diverted opioids and exacerbating the addiction crisis. They also noted that the “evidence base” behind safer supply was exceptionally poor and would not meet normal health-care standards.
Yet, critics of safer supply, and harm reduction radicalism more broadly, were often afraid to voice their opinions. The harm reductionists were institutionally and culturally dominant in the late 2010s and early 2020s, and opponents often faced activist harassment, aggressive gaslighting, and professional marginalization. A culture of self-censorship formed, giving both the public and influential policymakers a false impression of scientific consensus where none actually existed.
The resurgence in recovery-oriented strategies
Things changed in the mid-2020s. British Columbia’s failed drug decriminalization experiment eroded public trust in harm reductionism, and the scandalous failures of safer supply—and supervised consumption sites, too—were widely publicized in the national media.1
Whereas harm reductionism was once so powerful that opponents were dismissed as anti-scientific, there is now a resurgent interest in alternative, recovery-oriented strategies.
These cultural shifts have fuelled a more fractious, but intellectually honest, national debate about how to tackle the overdose crisis. This has ruptured the institutional dominance enjoyed by harm reductionists in the addiction medicine world and allowed their previously silenced opponents to speak up.
When I first attended CSAM’s annual scientific conference two years ago, recovery-oriented critics of radical harm reductionism were not given any platforms, with the exception of one minor presentation on safer supply diversion. Their beliefs seemed clandestine and iconoclastic, despite seemingly having wide buy-in from the addiction medicine community.
While vigorous criticism of harm reductionism was not a major feature of this year’s conference, there was open recognition that legitimate opposition to the movement existed. One major presentation, given by Dr. Didier Jutras-Aswad, explicitly cited safer supply and involuntary treatment as two foci of contention, and encouraged harm reductionists and recovery-oriented experts to grab coffee with one another so that they might foster some sense of mutual understanding.2
Is this change enough?
While CSAM should be commended for encouraging cross-ideological dialogue, its efforts, in this respect, were also superficial and vague. They chose to play it safe, and much was left unsaid and unexplored.
Two addiction medicine doctors I spoke with at the conference—both of whom were critics of safer supply and asked for anonymity—were nonplussed. “You can feel the tension in the air,” said one, who likened the conference to an awkward family dinner where everyone has tacitly agreed to ignore a recent feud. “Reconciliation requires truth,” said the other.
One could also argue that the organization has taken an inconsistent approach to encouraging respectful dialogue. When recovery-oriented experts were being bullied for their views a few years ago, they were largely left on their own. Now that their side is ascendant, and harm reductionists are politically vulnerable, mutual respect is in fashion again.
When I asked to interview the organization about navigating dissension, they sent a short, unspecific statement that emphasized “evidence-based practices” and the “benefits of exploring a variety of viewpoints, and the need to constantly challenge or re-evaluate our own positions based on the available science.”
But one cannot simply appeal to “evidence-based practices” when research is contentious and vulnerable to ideological meddling or misrepresentation.
Compared to other medical disciplines, addiction medicine is highly political. Grappling with larger, non-empirical questions about the role of drug use in society has always necessitated taking a philosophical stance on social norms, and this has been especially true since harm reductionists began emphasizing the structural forces that shape and fuel drug use.
Until Canada’s addiction medicine community facilitates a more robust and open conversation about the politicization of research, and the divided—and inescapably political—nature of their work, the national debate on the overdose crisis will be shambolic. This will have negative downstream impacts on policymaking and, ultimately, people’s lives.
Our content is always free – but if you want to help us commission more high-quality journalism,
consider getting a voluntary paid subscription.
armed forces
Why Do Some Armed Forces Suffer More Suicides Than Others?

Any single suicide is an unspeakable tragedy. But public health officials should be especially alarmed when the numbers of suicides among a particular population spike. Between 2019 and 2023, the suicide rate across Canada fell from 12.3 per 100,000 to 9.5 per 100,000. U.S. numbers aren’t that different (although they’re heading in the other direction).
Holding public officials and institutions accountable using data-driven investigative journalism.
Against this context, the suicide rate among active Canadian military personnel is truly alarming. Data included in a 2021 Report on Suicide Mortality in the Canadian Armed Forces (CAF) showed that the three year moving average annual rate for suicides in all services of the CAF was 23.38 per 100,000 – around twice the national rate. Which, of course, is not to ignore the equally shocking suicide rates among military veterans.
This isn’t specific to Canada. All modern military communities have to worry about numbers like those. Officials in the Israel Defense Force – now hopefully emerging from their longest and, by some measures, costliest war ever – are struggling to address their own suicide crisis. But there’s a significant difference that’s probably worth exploring.
Through 2024, 21 active duty IDF soldiers took their own lives. This dark number has justifiably inspired a great deal of soul searching and, naturally (it being Israel), finger pointing. But the real surprise here is how low that number is.
It’s reasonable to estimate that there were 170,000 active duty soldiers in the IDF during 2024 and another 300,000 active reservists. If you count all of those together, the actual suicide rate is just 4.5 per 100,000 – which is less than half of the typical civilian suicide rate in Western countries!
Tragic. But hardly an epidemic. Those soldiers have all lost friends and faced battlefield conditions that I, for one, find impossible to even comprehend. And those 300,000 reservists? They’ve been torn away from their families, businesses, and normal lives for many months. Many have suffered devastating financial, social, and marital pressures. And still: we’re losing them at lower rates than most civilian populations!
Is there any lesson here that could help inform CAF policy?
One obvious difference is sense of purpose: IDF members are fighting for the very existence of their people. They all saw and felt the horrors of the October 7 massacres and know that there are countless thousands of adversaries who would be happy do it again in a heartbeat¹. And having a general population that overwhelmingly supports their mission can only help that sense.
But there are some other factors that could be worth noting:
- The IDF is unusual in that it subjects all potential conscripts to mandatory psychological screening – resulting in many exemptions.
- Small, stable units are intentionally kept together for years. In fact, units are often formed from groups who have known each other since their early school years. This cohesion also helps with post-service integration.
- Every IDF battalion has a dedicated officer trained in brief interventions and utilization rates are high.
Is there anything here that CAF officials could learn from?
-

 armed forces2 days ago
armed forces2 days agoCanadian veteran says she knows at least 20 service members who were offered euthanasia
-

 Business2 days ago
Business2 days agoCarney shrugs off debt problem with more borrowing
-

 Frontier Centre for Public Policy1 day ago
Frontier Centre for Public Policy1 day agoRichmond Mayor Warns Property Owners That The Cowichan Case Puts Their Titles At Risk
-

 National2 days ago
National2 days agoConservative bill would increase penalties for attacks on places of worship in Canada
-

 Daily Caller1 day ago
Daily Caller1 day agoLaura Ingraham’s Viral Clash With Trump Prompts Her To Tell Real Reasons China Sends Students To US
-

 Business1 day ago
Business1 day agoSluggish homebuilding will have far-reaching effects on Canada’s economy
-

 Automotive2 days ago
Automotive2 days agoThe high price of green virtue
-

 Bruce Dowbiggin2 days ago
Bruce Dowbiggin2 days agoMaintenance Mania: Since When Did Pro Athletes Get So Fragile?












