Community
Conservative MP Leslyn Lewis condemns MAiD in Parliament as targeting nation’s most vulnerable

From LifeSiteNews
‘I call upon with government to reverse its course and instead provide help and hope for Canadians suffering with mental health conditions’
Conservative MP Leslyn Lewis condemned the Trudeau government’s treatment of Canada’s most vulnerable, revealing that 36 Canadians are euthanized every day.
On November 28, Dr. Leslyn Lewis, Conservative Member of Parliament (MP) for Haldimand-Norfolk, Ontario, addressed Parliament on the dangers of Medical Assistance in Dying (MAiD), the euphemistic name for Canada’s euthanasia regime.
“The poor, homeless, the abused, veterans, seniors, youth, adults suffering with disabilities, those suffering with depressions, and mental health conditions,” Lewis said. “These are among the most vulnerable in our society that are falling through the cracks of Canada’s Medical Assistance in Dying regime.”
The most vulnerable are falling through the cracks of Canada's Medical Assistance in Dying regime.
Every day 36 Canadians die by MAiD, the HIGHEST NUMBER in the world. Canadians suffering with mental illness need help and hope, not euthanasia. This gov't must reverse course. pic.twitter.com/tT8x5PBpxq
— Dr. Leslyn Lewis (@LeslynLewis) November 28, 2023
“They are the ones who will be at risk when the MAiD laws in Canada are expanded in March 2024,” the pro-life MP added. “Last year, death by euthanasia increased by 30 percent from the year before. Every day in Canada, 36 people use MAiD to end their lives, which is the highest in the world.”
“I call upon with government to reverse its course and instead provide help and hope for Canadians suffering with mental health conditions,” Lewis appealed.
On March 9, 2024, MAiD is set to expand to include those suffering solely from mental illness. This is a result of the 2021 passage of Bill C-7, which also allowed the chronically ill – not just the terminally ill – to qualify for so-called doctor-assisted death.
The mental illness expansion was originally set to take effect in March of this year. However, after massive pushback from pro-life groups, conservative politicians and others, the Liberals under Trudeau delayed the introduction of the full effect of Bill C-7 until 2024 via Bill C-39.
The expansion comes despite warnings from top Canadian psychiatrists that the country is “not ready” for the coming expansion of euthanasia to those who are mentally ill, saying expanding the procedure is not something “society should be doing” as it could lead to deaths under a “false pretense.”
Similarly, Angelina Ireland, the head of one of Canada’s few pro-life hospice societies, recently warned that euthanasia has become a national “horror” show.
“Unfortunately, there is no reprieve in sight as think Medical Assistance in Dying (MAiD) becomes a national horror and the ‘professionals’ sharpen up their needles,” Ireland told LifeSiteNews.
“We have reached the point where we must all protect each other from MAiD,” she noted.
Euthanasia deaths have gone through the roof in Canada since it became legal in 2016.
According to Health Canada, in 2022, 13,241 Canadians died by MAiD lethal injection, which is 4.1 percent of all deaths in the country for that year, and a 31.2 percent increase from 2021.
The number of Canadians killed by lethal injection since 2016 now stands at 44,958.
Community
Support local healthcare while winning amazing prizes!
|
|
|
|
|
|
Community
The 2025 Red Deer Hospital Lottery is here! Lower ticket prices!!

|
|
|
|
|
|
-
 Business6 hours ago
Business6 hours agoRFK Jr. says Hep B vaccine is linked to 1,135% higher autism rate
-

 Alberta1 day ago
Alberta1 day agoAlberta Independence Seekers Take First Step: Citizen Initiative Application Approved, Notice of Initiative Petition Issued
-
 Crime19 hours ago
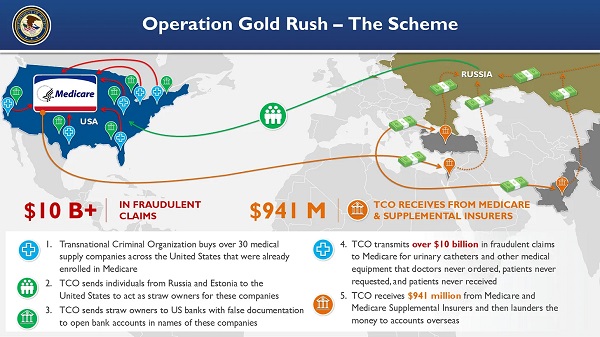
Crime19 hours agoNational Health Care Fraud Takedown Results in 324 Defendants Charged in Connection with Over $14.6 Billion in Alleged Fraud
-

 Crime1 day ago
Crime1 day agoSuspected ambush leaves two firefighters dead in Idaho
-

 Health19 hours ago
Health19 hours agoRFK Jr. Unloads Disturbing Vaccine Secrets on Tucker—And Surprises Everyone on Trump
-

 Alberta1 day ago
Alberta1 day agoWhy the West’s separatists could be just as big a threat as Quebec’s
-

 Business1 day ago
Business1 day agoCanada Caves: Carney ditches digital services tax after criticism from Trump
-

 Business1 day ago
Business1 day agoMassive government child-care plan wreaking havoc across Ontario






